Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
The Mechanics of Respiration
The Mechanics of Respiration
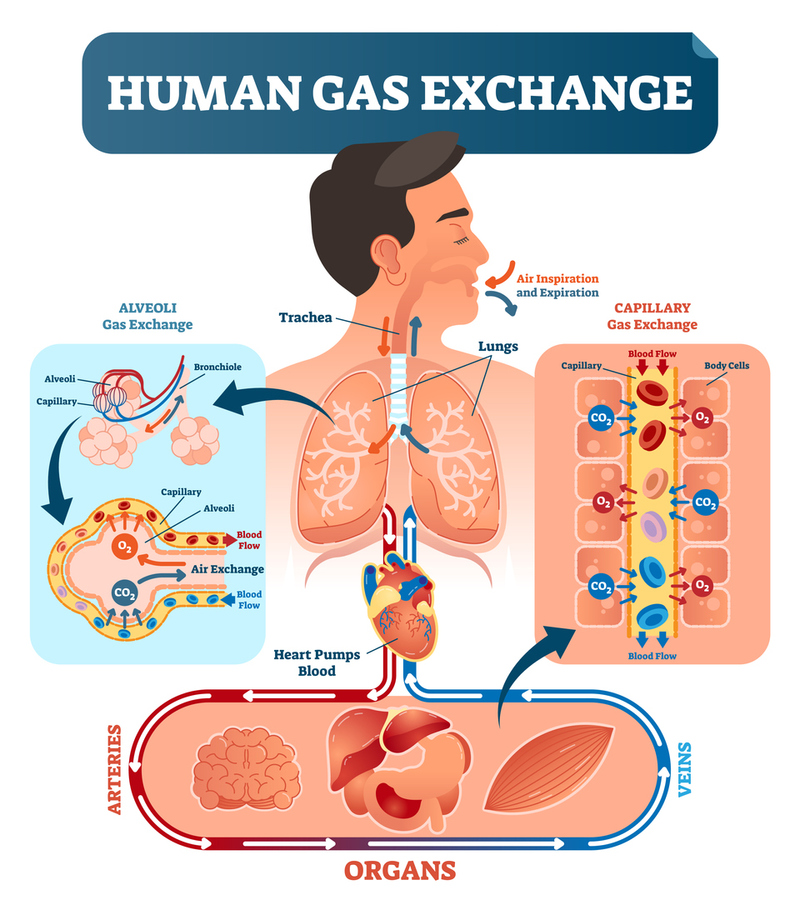 The term "respiration" has different colloquial and medical meanings. In normal conversation, it refers to breathing, the movement of air in and out of the lungs. In medicine, the process of moving air is called ventilation. Respiration is specifically the exchange of oxygen and carbon dioxide inside the alveoli of the lungs. This section will delve deeper into the differences between respiration and ventilation along with the many details about the two that are commonly tested on the national registry exams.
The term "respiration" has different colloquial and medical meanings. In normal conversation, it refers to breathing, the movement of air in and out of the lungs. In medicine, the process of moving air is called ventilation. Respiration is specifically the exchange of oxygen and carbon dioxide inside the alveoli of the lungs. This section will delve deeper into the differences between respiration and ventilation along with the many details about the two that are commonly tested on the national registry exams.
Respiration vs. Ventilation
Respiration and ventilation are two different things. Ventilation is mechanical and involves the movement of air. Respiration is physiologic and involves the exchange of gases in the alveoli (external respiration) and in the cells (internal respiration).
- RESPIRATION: The exchange of oxygen and carbon dioxide.
- VENTILATION: The mechanical drawing in and expelling out air via breathing.
- OXYGENATION: Oxygen dissolved in blood and body fluids; specifically, this is the process of loading oxygen molecules onto hemoglobin molecules in the bloodstream.
In order to respirate, a patient must have adequate ventilation. However, the reverse is not true. Just because a patient is ventilating does not mean respiration is occurring. This is because the systems for moving air and absorbing gases from that air are separate. This commonly happens when blood flow is reduced to the lungs, or the alveoli are filled with fluid (pneumonia, drowning, etc.) In rare cases, internal (cellular) respiration can be disrupted by toxins and certain rare medical conditions.
Ventilation
As mentioned above, ventilation is the movement of air through the respiratory tract. The process of ventilation is further broken down into mechanical ventilation and alveolar ventilation.
MECHANICAL VENTILATION: Mechanical ventilation is the movement of air from the outside environment in and out of the lungs. It occurs in two major phases the active phase and the passive phase:
- Active phase--when the diaphragm contracts and the chest expands, drawing air into the lungs.
- The thoracic wall expands outward and the diaphragm flexes downwards, creating a negative pressure that pulls air into the lungs.
- As air is sucked in the pressure in the chest (intrathoracic pressure) rises until the lungs have excess pressure leading to the passive phase.
- Passive phase--the relaxation of the diaphragm, which allows for the air to be exhaled.
- The diaphragm and other muscles of breathing relax
- The spring-like nature of the lung tissue passively pulls the lungs together like a balloon, forcing air out of the lungs and into the airway.
The respiratory system moves air through pressure gradients created by the diaphragm. If the pleural cavity is breached, these pressure gradients collapse and the pressure within and outside the chest becomes equal (equilibration). Depending on the size of the breach, this makes the inhalation process much more difficult or--in severe cases--nearly impossible.
Mechanical ventilation is controlled by the phrenic nerve which signals the diaphragm to contract, this occurs both automatically in response to the body's level of oxygen and CO2--via signals from the hypothalamus--and voluntarily when an individual consciously focuses on their rate of breathing.
ALVEOLAR VENTILATION: is defined as the amount of air that reaches the alveoli and is available for gas exchange with the blood. Many factors affect alveolar ventilation. Knowing the factors that exist is important, but remembering each definition is not.
- Tidal Volume = the amount of air inhaled in one breath.
- Dead Space = the portion of the airway in which no gas exchange takes place.
- Vital Capacity = the maximum amount of air a person can expel from the lungs after maximum inhalation.
- Respiratory Rate = the number of breaths per minute.
- Minute Volume = the volume of gas inhaled or exhaled from a person’s lungs per minute.
- Residual Volume = the amount of air remaining in the lungs after a maximum expiratory effort.
Respiration
As mentioned above, respiration is the actual exchange of gases in both the lungs and the cells. The process of respiration is controlled by complex hormonal and neural signaling, which detects concentrations of oxygen and CO2, and acts to alter the amount of blood flow through the capillaries or the size of the smooth muscle bronchioles which connect the alveoli to the rest of the airway.
EXTERNAL RESPIRATION: Within the alveoli, oxygen from the air diffuses across the thin cell membrane and attaches to the red blood cells, which have a low concentration of oxygen. At the same time, the carbon dioxide-rich deoxygenated red blood cells release carbon dioxide, which diffuses across the cell membrane to the area of a lower carbon dioxide concentration (the inspired air in the lungs), for expiration.
INTERNAL RESPIRATION: The cells exchange gases with the red blood cells in the capillaries in the same manner as the alveoli exchange gases. When this occurs in the cells, it is known as "internal respiration," as there is no exchange of gases with the environment outside the body.
Carbon dioxide is either attached to hemoglobin or dissolved in blood plasma as part of the bicarbonate buffer system. These storage systems allow carbon dioxide to be exhaled by the lungs (hemoglobin detachment) or excreted by the kidneys (dissolved in plasma as part of the buffer system).