Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
CPR in the Infant
CPR in the Infant
CPR is used to maintain blood flow through the body in the event of cardiac arrest. This has a dual function, it provides oxygen to vital tissues such as the brain, which rapidly dies without oxygen and increases the preload reaching the right side of the heart which stimulates it to resume beating.
Infants have different needs than adults, they have a dramatically higher healthy respiratory rate and heart rate. Balancing these needs is the reason why the recommendations for CPR in infants differ from that of adults and children.
Remember, Scene safety is paramount in all situations, even a cardiac arrest. Ensure that you and your team is safe prior to attempt any rescue!
The C.A.B Protocol for CPR in Infants
An infant is a patient that is under 1 year of age, each element of CPR has significant differences from the adult protocol. In summary, the compression rate is higher, the breath rate is higher, and the ratio of breaths to compressions changes based on the number of rescuers.
Circulation
As with adults, the quality of chest compressions is the greatest determinant of patient outcome. You should be depressing the chest approximately 1/3 of its anteroposterior diameter. In practice, you will need to press just slightly harder than you will feel is appropriate.
As opposed to adults a rate around 120 beats per minute is preferred to the usual 100.
Given the small size of the chest alternative compression techniques are needed. The 2-thumb technique is done by holding the infant underneath the arms, using both thumbs to compress the chest and the rest of the fingers to support the back of the infant. The 2-finger technique is done by placing the infant flat on a surface, putting 2 fingers on the chest and using the 2 fingers of the other hand to support the fingers on the chest.
AED's will also have specialized pediatric pads that are usually placed on the front and back of the infant as opposed to the left side and front chest as in an adult or older child.
Note that in neonatal patients chest compressions should be considered if the heart rate is below 60bpm in addition to the usual chest compressions with an absent pulse! Before beginning chest compressions in a bradycardic neonate, you must ensure they are well ventilated. Providing positive pressure ventilation will often increase the heart rate to an acceptable level.
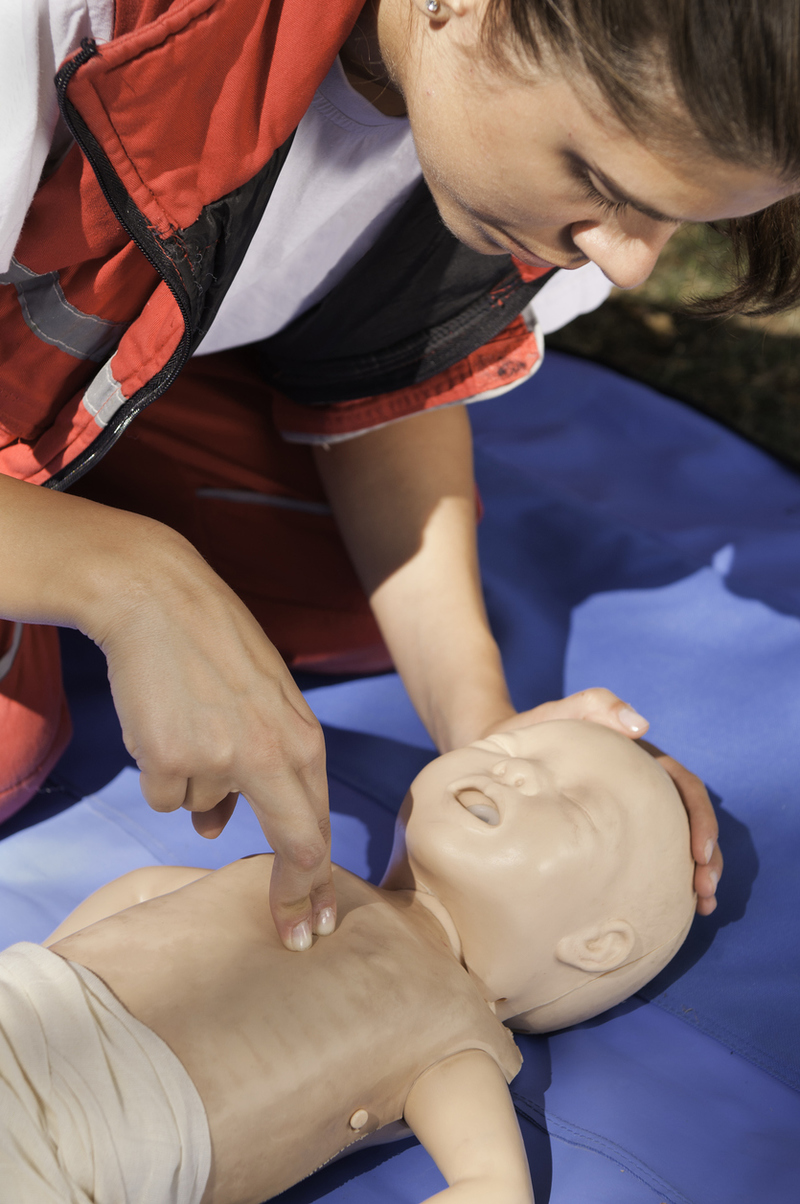
Airway
As with adults you will use the "sniffing position" with the head tilted back and the chin forward to open the airway, as opposed to adults tilting the head too far back can occlude the airway, so ensure that chest rise is occurring with each breath.
Have a suction device ready as excessive secretions and vomiting are common in this age group
Breathing
Again, just as in adults, you will deliver breaths with a barrier device or bag-valve-mask. Ensure that you are using an infant-sized bag! Using an adult or pediatric bag in an infant can cause significant lung trauma.
With premature or small infants or when you are using "mouth to mouth" with a one-way mask, ensure that you stop squeezing the bag when the chest stops rising to minimize the potential for damage to the lungs.
Remember that with infants and children, the compression-to-breath ratio changes when more than one rescuer is involved. Provide 30 compressions per 2 breaths (30:2) if you are alone, but if you are with a partner, deliver 15 compressions followed by 2 breaths (15:2). This is an essential testing point that is often encountered on exams.
Single Rescuer CPR
Responsive or Unresponsive
First, determine if the patient is responsive or not via rubbing the sternum or providing firm palm slaps to the infant's back. If they respond, evaluate for any other potential life threats. If there is no response, check for a pulse at the carotid. Activate the emergency response system by radioing for ACLS support and if available, obtain an AED.
Pulse Check
If unresponsive, simultaneously check for a carotid pulse and visible breathing via chest rise for no more than 10 seconds. Note that Gasping or grunting is not breathing.
- Definite pulse + inadequate breathing: 1 rescue breath 2-3 seconds.
- Definite pulse + breathing effectively: monitor until ALS unit arrives.
- Pulseless or pulse below 60bpm + apneic: remove clothes from the chest and begin CPR.
- BEGIN compressions if pulse is less than 60 beats per minute in infants.
Get an AED
The AED will guide you through each step once powered on. Be sure to listen carefully to each command and follow accordingly. Each AED has defibrillator pads. Follow the instructions and utilize the pictures on the pads if you forget placement. Though not ideal, adult pads can be used by placing one on the front of the infant and another between the shoulder blades.
AED's are becoming increasingly available to EMS services and the public. Nearly all BLS teams will carry an AED, if one is not available in your ambulance there will often be AED's available in many public places such as malls, airports, gyms, college campuses, and retirement homes.
If it is not immediately obvious where to obtain an AED, you should activate the emergency response, initiate CPR, and specifically instruct one or more bystanders to search for an AED.
For witnessed cardiac arrest, attach the AED pads to the patient’s bare chest. Do not touch the patient during this time as the AED is determining if a shock is advised. If a shock is not advised, quickly begin high-quality chest compressions for 2 minutes and recheck a rhythm every 2 minutes until an ALS crew arrives or the patient begins to move. The AED should prompt you to do this.
Shock Advised
If a shock is indicated, resume compressions while the AED is charging.
AED's will not deliver a shock until the button is pressed, as a matter of safety, the individual giving chest compressions at that moment should be the one to press the shock button. Once the AED has charged, STAND CLEAR then press the button to deliver the shock. Immediately resume chest compressions for 2 minutes. The AED prompts you when to stop to re-analyze the rhythm.
Dual Rescuer CPR vs. Single Rescuer CPR
Unlike newer adult guidelines where a 30:2 compression ratio is always recommended. In pediatric patients, the use of a 15:2 ratio is called for when a second rescuer is present. This is due to the increased need of oxygen for younger patients and the lower circulating blood volume.
- Additionally, the 2nd rescuer may:
- activate the emergency response system;
- be an extra set of eyes for scene safety;
- obtain the AED and first aid kit;
- attach AED pads while breaths are being administered between compressions;
- alternate every 2 minutes in performing high-quality chest compressions;
- perform pulse checks when indicated by the AED;
- encourage you to do better chest compressions, ensuring high-quality CPR;
- assist in other tasks as needed to optimize patient survival.
Be sure to assign responsibilities and stick with them. Communication is key here. No one wins a prize for being a "better rescuer." Someone's life depends on you working together as a TEAM.