Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
CPR in the Adult Patient
Category: Cardiology
Topic: Basic Life Support
Level: EMR
Next Unit: CPR in the Infant
23 minute read

CPR in the Adult Patient
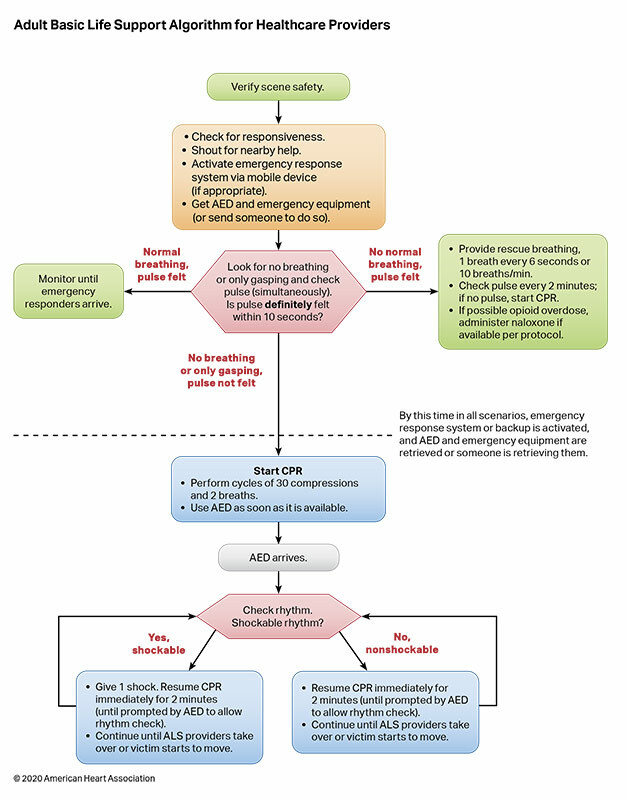
- Cardiopulmonary Resuscitation (CPR) is a critical intervention that can save a person's life in cardiac arrest. The cornerstone of cardiac arrest management is effective and timely CPR. Early bystander CPR can double or even triple the chances of survival for a person in cardiac arrest, making it crucial to start CPR immediately, without delay. CPR restarts or maintains blood flow and oxygenation to vital organs. Early recognition and activation of emergency medical services (EMS) are critical for improving patient outcomes in cardiac arrest.
- CPR pushes blood through the body and increases the preload reaching the right side of the heart, further stimulating it to resume beating.
This section will review CPR using the algorithm CAB, a rearrangement of the ABCs proposed by the American Heart Association, given the importance of initiating CPR rapidly if no pulse is present.
Remember, Scene safety is paramount in all situations, even a cardiac arrest. Ensure that you and your team are safe before attempting any rescue!
The CAB Protocol for CPR in Adults
The CAB protocol for CPR in adults is a rearrangement of the traditional EMS ABCs (Airway, Breathing, Circulation) that better meet the needs of a patient unconscious and suspected of being in cardiac arrest. The placement of "C" at the front of the acronym is meant to communicate that effective and uninterrupted chest compressions are the most vital intervention in this patient population. Follow that by positioning the airway to allow for maximal airflow and the delivery of effective rescue breaths.
Circulation
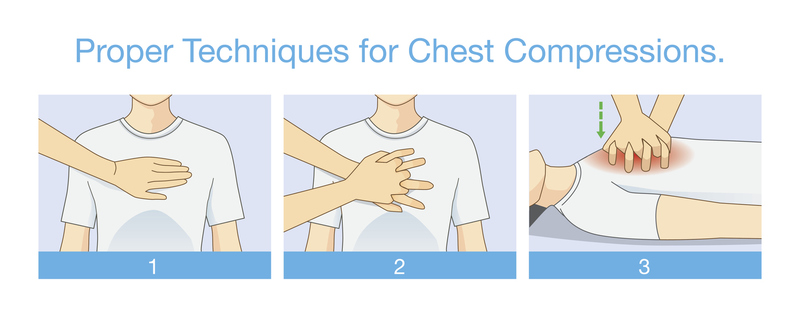
- The heart is an automated pump that moves all your blood around. When the heart stops beating, blood flow to the body stops, and vital organs like the brain are deprived of oxygen. By performing chest compressions, the rescuer acts as a manual pump, keeping blood flowing to the vital organs until the heart can be restarted.
- Chest compressions are delivered at a rate of 100-120 compressions per minute, over the mid-sternum, to a minimum depth of 2 inches. For a patient that does not have an advanced airway in place, you will deliver 30 compressions before giving 2 rescue breaths from a bag valve mask; this is known as a 30:2 ratio. If a patient has been intubated or had an advanced airway placed by an ACLS provider, you will provide continuous chest compressions as pausing for breaths is no longer required to deliver effective ventilation.
- Every 2 minutes of CPR, check for a pulse. Attach an AED as soon as it becomes available; it is best to wait for the natural pause between cycles of CPR while breaths are being delivered.
Airway
After every 30 compressions in an un-intubated patient, deliver 2 rescue breaths.
The patient should be placed in the "sniffing position" with the head tilted back, and the chin lifted upwards. Two full breaths are delivered by bag valve mask with 1 second in between each breath. Watch for chest rise to ensure the ventilations are effective. Dual rescuer CPR is more effective as it allows you to maintain this position and not have to reset the patient's airway in between cycles.
Breathing
As above, two breaths are delivered after every 30 compressions via a bag valve mask connected to 100% oxygen. If a bag valve mask is not available, use a barrier mask with a one-way valve to deliver "mouth-to-mouth" breaths. Remember, never be without a barrier device for CPR. Position the airway to allow for maximal airflow and the delivery of effective rescue breaths.
Single Rescuer CPR
Responsive vs. Unresponsive
First, determine if the patient is responsive or not via a good shout of "ARE YOU OK?" then firmly tap on their shoulders. If they respond, evaluate for any other potential life threats. If there is no response, move to check for a pulse. Activate the emergency response system by radioing for ACLS support and if available, obtain an AED.
Pulse Check
If unresponsive, simultaneously check for a carotid pulse and visible breathing via chest rise for no more than 10 seconds. Note that Gasping or grunting is not breathing.
- Definite pulse + inadequate breathing: 1 breath every 6 seconds or 8-10 breaths/min.
- Definite pulse + breathing effectively: monitor until an ALS unit arrives.
- Pulseless + apneic: remove clothes from the chest and begin CPR.
Begin Chest Compressions:
If there is no pulse and no breathing: Position the victim on their back, kneel beside the victim, place the heel of one hand on the center of the chest, place the other hand on top of the first, and interlock your fingers. Press down on the chest with your body weight to a depth of at least 2 inches, and allow the chest to recoil completely after each compression.
Give rescue breaths:
Tilt the victim's head back and lift the chin. Pinch the victim's nose closed, take a deep breath, and give 2 breaths over 1 second each, watching for chest rise. After every 30 compressions, tilt the patient's head back and lift the chin to deliver 2 rescue breaths. Watch for chest rise to ensure the breaths are effective.
Get an AED
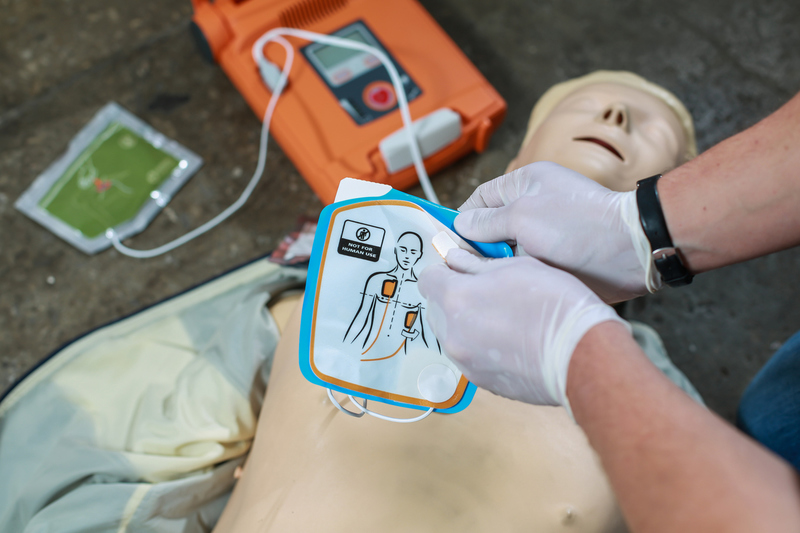
The AED will guide you through each step once powered on. Be sure to listen carefully to each command and follow accordingly. Each AED has defibrillator pads. Follow the instructions and utilize the pictures on the pads if you forget placement. It is crucial to attach the AED as soon as possible to improve the chances of survival.
It is crucial to check the expiration date of the AED pads and battery and to maintain the AED properly. AEDs are becoming increasingly available to EMS services and the public. Nearly all basic life support (BLS) teams carry an AED. If one is not available in your ambulance, there will often be AEDs available in many public places such as malls, airports, gyms, college campuses, and retirement homes.
If it is not immediately obvious where to obtain an AED, you should activate the emergency response, initiate CPR, and specifically instruct one or more bystanders to search for an AED.
For a witnessed cardiac arrest, attach the AED pads to the patient's bare chest. Do not touch the patient during this time as the AED is determining if a shock is advised. If a shock is not advised, quickly begin high-quality chest compressions for 2 minutes and recheck a rhythm every 2 minutes until an ALS crew arrives or the patient begins to move. The AED should prompt you to do this.
Shock Advised!
If a shock is indicated, resume compressions while the AED is charging.
AEDs will not deliver a shock until the button is pressed. As a matter of safety, the individual giving chest compressions at that moment should be the one to press the shock button. Once the AED has charged, STAND CLEAR! Then, press the button to deliver the shock. Immediately resume chest compressions for 2 minutes. The AED prompts you when to stop to re-analyze the rhythm.
Continue CPR: Continue chest compressions and rescue breaths until help arrives or the victim shows signs of life.
Dual Rescuer CPR vs. Single Rescuer CPR
It is recommended to use a 30:2 ratio for ALL adult CPR, regardless of whether a second rescuer is present. Minimizing the interruption of high-quality chest compressions is the most important factor in the survival of cardiac arrest.
If a second rescuer is present, they may:
- Activate the emergency response system
- Be an extra set of eyes for scene safety
- Obtain the AED and first aid kit
- Attach AED pads while breaths are being administered between compressions
- Alternate every 2 minutes in performing high-quality chest compressions
- Perform pulse checks when indicated by the AED
- Encourage the primary rescuer to perform better chest compressions, ensuring high-quality CPR
Assist in other tasks as needed to optimize patient survival. Assign responsibilities and communicate effectively as a team. Remember, no one wins a prize for being a "better rescuer." Someone's life depends on you working together!
Dual rescuer CPR is more effective than single rescuer CPR as it allows for more consistent and effective chest compressions and ventilation. The second rescuer can help with tasks such as activating the emergency response system, obtaining the AED and first aid kit, and alternating every 2 minutes in performing high-quality chest compressions. Communication is key in dual rescuer CPR, and it is important to assign responsibilities and stick with them to optimize patient survival.
The compression-to-breath ratio remains 30:2 for all adult CPR, regardless of whether one or two rescuers are present. The second rescuer may assist with ventilation by providing bag valve mask ventilation while the primary rescuer performs chest compressions. The second rescuer can also help maintain the airway and position the patient.
Be sure to assign responsibilities and stick with them. Communication is key here. No one wins a prize for being a "better rescuer." Someone's life depends on you working together as a TEAM.