Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Trauma During Pregnancy
Category: Trauma
Topic: Special Considerations in Trauma
Level: EMT
Next Unit: Pediatric Trauma Patients
14 minute read
EMS providers should recognize that pregnant women who have suffered an injury should be evaluated by a physician in the emergency room. If the pregnant woman is having any symptoms related to shock, high-concentration oxygen should be administered.
KEEP LEFT!
Pregnant women in the third trimester should be placed on their left side
If a pregnant patient is placed on a spine board, it should be tilted to the left after the patient is fully secured. Left-leaning takes the weight of the pregnant uterus off of the slightly right-of-the-midline aorta and--especially--the vena cava, which has less wall musculature and is more susceptible to compression.
Vena cava compression → decreased blood to the right side of the heart → less oxygenation (right heart) and stroke volume (left heart) → maternal hypotension → less oxygenation to the placenta → fetal hypoxia → fetal distress.
►Patient nausea is the "canary in the mine." If a maternal patient begins to get nauseated, don't write it off as "Well, they're pregnant, so that's normal." You should suspect something may have changed, such as their hemodynamic status, and reevaluate them and their condition.
Pregnant patients can sustain all types of trauma and are especially susceptible to falls and physical abuse.
Trauma Effects Roll Downhill: Effects on Fetal Health
Trauma to expectant mothers can have effects on fetal health.
Normally, the changes that pregnant patients undergo that are important during trauma include
- cardiovascular changes and
- decreased gastrointestinal motility.
CARDIOVASCULAR:
- Cardiovascular changes may include an increase in total vascular volume and an increase in maternal heart rate in the third trimester, making shock in a third-trimester patient difficult to detect.
- Third-trimester fetus size can affect venous return in pregnant patients lying flat on their backs. [SEE ABOVE]
GI: Decreased gastrointestinal motility increases the risk of vomiting and aspiration after trauma.
Fetal Distress
Fetal distress can be caused due to hypoxia or hypovolemia/shock of the pregnant mother.
- ABRUPTIO PLACENTAE: Separation of the placenta from the uterine wall may be a complication of trauma in the pregnant patient and may present with abdominal pain and often presents with vaginal bleeding. This separation carries a high risk of fetal death. The force of a trauma associated with abruption is due to the shearing away from the uterine wall at the placental/maternal interface there. Arteries are disrupted and bleeding is brisk.
- Fetal injury in pregnant patients can also be caused by penetrating trauma, trauma from seat belts, and cardiac arrest due to trauma. Any penetrating injury (knife, GSW) in the abdomen should be assumed to involve the fetus.
- During traumatic incidents involving a pregnant patient, EMS providers must remember that there are actually two patients to assess. However...The most common cause of fetal death in maternal trauma is maternal death. Therefore, your primary focus is the mother.
- Internal blood loss is difficult to assess in pregnant patients due to the signs of shock often being masked. This means that when signs of shock are apparent, your patient is further into the downward spiral than she appears!
Management
EMS providers should treat the pregnant patient aggressively in the face of severe trauma.
IMMOBILIZATION: The pregnant patient with suspected spinal injury should be immobilized to a long spine board, with the board tilted to the left after properly securing the patient.
VAGINAL EXAM = HANDS OFF! The need for a vaginal exam may be present in pregnant patients involved in trauma, check for crowning if indicated but this is best performed at the receiving facility.
In the field, the only indication for a vaginal exam is to determine whether the baby is delivering, and that can be done by direct inspection.
FUNDAL HEIGHT: The size of the fetus (age of gestation in weeks) is important during the assessment of the pregnant patient involved in trauma, but it is difficult to assess the fetus. 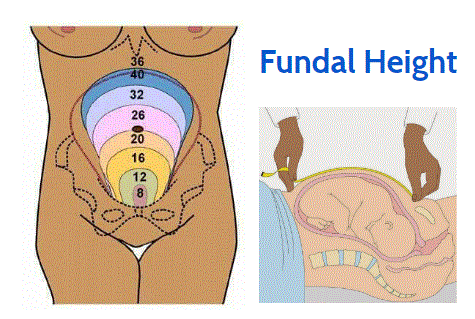
- If you can feel the pregnant uterus through the abdomen, the patient is at least in her second trimester (12 weeks and beyond).
- The top convexity of the uterus (the fundal "height") reaches the umbilicus at 20 weeks (halfway through the pregnancy of 40 weeks).
For every fingerbreadth above or below the umbilicus, you can add or subtract a week of gestation. However, this only applies within 5 fingerbreadths. For example, if the fundal height is 2 fingerbreadths below the umbilicus, she is probably 18 weeks gestation (out of 40). If 3 fingerbreadths above...23 weeks. Below 15 weeks and above 25 weeks, the inaccuracy makes this "guestimate" completely ineffective. All you can say above the umbilicus + 5 fingerbreadths is that she is most likely in her 3rd trimester.
- Twins will throw this whole brilliant scheme off. If she's had prenatal care, she'll know if she has more than one baby; if she hasn't, anything's possible!
ABCs: During the management of pregnant trauma patients, EMS providers should
- manage the airway and anticipate vomiting (have suction available),
- assure bilateral breath sounds are present, keeping oxygenation levels high by administering oxygen via non-rebreather (100% SPO2), and assist ventilations if breathing is inadequate
- circulation should be managed in the same way as other adult patients.
TRANSPORT:
- Transport the pregnant trauma patient on their left side.
- Consider ALS intercept or air medical resources in the event of major trauma to a pregnant patient.
- Inform the trauma center early of the impending transport of a pregnant trauma patient.