Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
The Physiological Response to Bleeding
The Physiologic Response to Bleeding
The body exists to keep oxygen and sugar flowing to the brain. The flow of blood is the most important element of the brain's physiology, so the physiology of blood loss is closely tied to the physiology of the brain.
Blood loss falls into one of two categories: compensated and decompensated. While blood loss is "compensated" when the body can alter other factors to keep the blood flow to the brain sufficient, it is "decompensated" when the loss of blood exceeds the ability of the heart and blood vessels to keep enough blood flowing to the brain.
This section will review how the body attempts to stop blood loss, how it compensates for low-volume blood loss, and what happens when the loss exceeds that compensation.
The Body's Response to Bleeding
The major factors that alter the body's response to blood loss are the rate of loss, age, and preexisting medical conditions. The young, old, and chronically ill are particularly susceptible to the effects of blood loss as their bodies have a reduced ability to either compensate for the loss or stop the loss of blood.
The immediate physiologic responses to bleeding are constriction of the blood vessels and the formation of clots. These two mechanisms work together to lower the amount of blood lost when a disruption in the wall of a blood vessel is detected by the body. Combined, these responses are known as "hemostasis."
Several things can disrupt hemostasis: clotting disorders, kidney/liver/spleen disease, medications for blood pressure/stroke/heart attack, and changes in temperature or hydration.
SYSTEMIC RESPONSE: 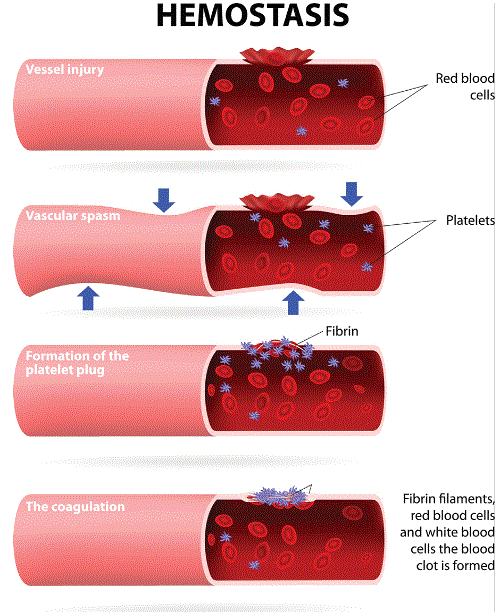
Hypoperfusion and Severe Blood Loss.
Hypoperfusion often results in the dysfunction of organs, known as shock. There are many types of shock, all involving insufficient blood flow, but the specific types related to bleeding are "hemorrhagic" and "hypovolemic" shock.
Shock varies in severity and the rate at which it progresses. In some patients, it may be barely noticeable for long periods of time, while in others, the onset of shock to clinical death can occur in minutes. In all patients, the major signs of entering shock are headache, fatigue, shortness of breath, excessive sense of calm, and heart rate changes.
Note that low blood pressure is not on the list. It is a sign of shock but cannot be relied upon for its detection. Hypotension is a late-stage finding, a sign that decompensation has already occurred and that the window to proactively treat shock has passed.
Management of Hypoperfusion and Shock
Excess blood loss prevents the heart from pumping correctly while also removing the fluid that carries oxygen to tissues. The combination of these two factors kills patients. Management of hypoperfusion due to blood loss focuses on maintaining the heart's ability to pump and reducing the amount of work it takes to move oxygen around the body.
Restoring the ability of the heart to pump is done by replacing the lost blood volume with other fluids. While saline cannot carry oxygen as red blood cells do, it is enough to stabilize patients who are beginning to enter shock due to low blood volume. Lowering the amount of work required to move oxygen is done by giving the patient oxygen via nasal cannula or non-rebreather mask. If the combination of fluids and oxygen do not stabilize the patient, giving blood products is an option that is routinely used in higher levels of care.
Always consider the need for more advanced forms of transport and the destination hospital the patient is being brought to. Patients with severe hypoperfusion due to blood loss as a result of trauma have up to a 25% higher chance of survival if treated at a designated trauma center.
General Assessment of Bleeding
 The PRIMARY SURVEY will focus on the identification of and management of life threats related to bleeding; this is a key element of circulation (C) in the ABCs of trauma. To fully assess circulation, you must evaluate the following: Heart rate, blood pressure, pulses in all extremities, capillary refill in all extremities, skin color/temperature, and the presence of any significant external wounds.
The PRIMARY SURVEY will focus on the identification of and management of life threats related to bleeding; this is a key element of circulation (C) in the ABCs of trauma. To fully assess circulation, you must evaluate the following: Heart rate, blood pressure, pulses in all extremities, capillary refill in all extremities, skin color/temperature, and the presence of any significant external wounds.
Reduced lung sounds and/or abdominal tenderness are other important physical exam findings, as they may indicate significant internal bleeding into the lung/abdominal spaces.
HIDDEN INJURIES: The presence of an injury that is hidden by clothing or patient position is a major potential contributor to possible internal/external blood loss and patient decompensation. Fully assessing all exterior surfaces of the patient is a crucial step in the evaluation of suspected blood loss!
MEDICAL HISTORY/PRE-EXISTING ILLNESSES: These are crucial for identifying things that can alter or mask signs and symptoms of bleeding patients; an accurate past medical history is vital. While knowledge of exact complicating conditions is not important, know that some medical conditions, as well as some medications, can mask the tachycardia/bradycardia, sweating, cyanosis, and cold skin that is seen in hemorrhagic shock. Always have a high index of suspicion for internal and external hemorrhage.
Some of the high-risk illnesses are myocardial infarction, stroke, diabetes, hemophilia, and pulmonary embolism.
Some of the high-risk medications are aspirin, blood pressure medication, and warfarin (coumadin).