Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
The Lungs and Pulmonary Capillaries
The Lungs and Pulmonary Capillaries
This section covers the anatomy of the lungs, including the structure of the organ, microscopic structures for gas exchange, and terms defining air movement through the lungs.
Inhaled air is split at the carina into left and right pathways. Each pathway is then subdivided into smaller paths that serve each individual lung lobe. These lobes are filled with countless alveoli and capillaries, which exchange gases in the blood for gases in the inhaled air.
The Structure of the Lung
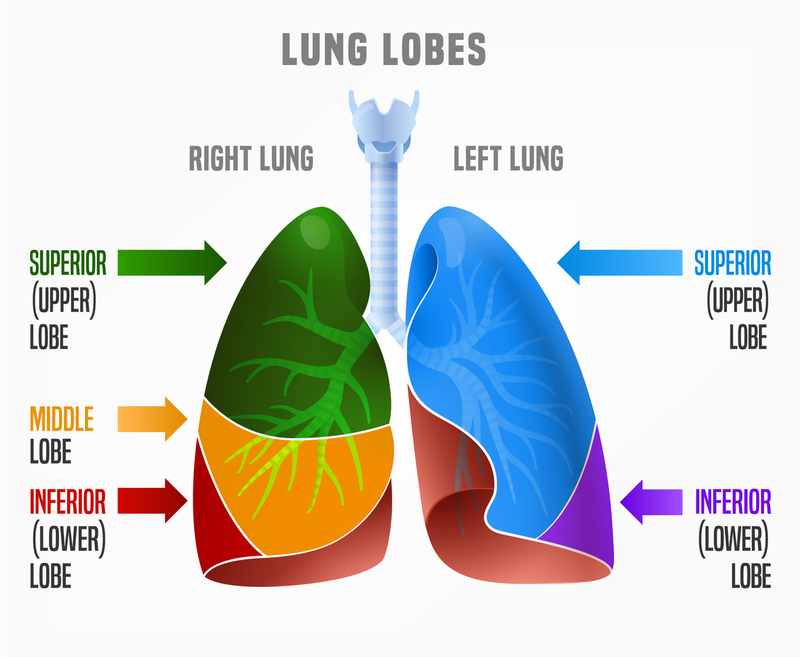
- Left Lung: Two lobes (upper and lower) and shares space with the heart.
- Right Lung: Three lobes (upper, middle, and lower).
- Mainstem Bronchi: The right mainstem bronchus is more vertical, making inhaled solids/fluids more likely to lodge in the right lung.
Other Structures of the Lung
PLEURA: The lungs are surrounded by delicate membranes named pleura.
- The visceral pleura is the inner membrane that covers the surface of each lung and dips into the spaces between the lobes.
- The parietal pleura is the outer membrane that is attached to the inner surface of the thoracic (chest) cavity. This pleura also separates the pleural cavity from the mediastinum (which houses the heart and the great vessels).
Serous fluid lies between the two membranes, allowing them to slide over each other without friction. This ensures that the lungs can easily inflate and deflate with minimal resistance.
HILUS: Each lung also has a hilus, an indentation in the surface where the blood vessels, bronchi, and nerve fibers enter and exit. The pulmonary hila (plural for hilus) are located on each lung's mediastinal (centermost) surface.
Gas Exchange Structures
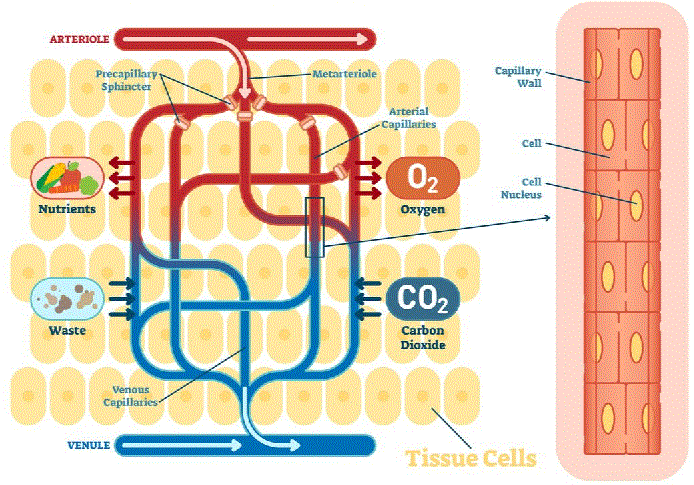
ALVEOLI: The alveoli collect oxygen from inhaled air and transfer it to the deoxygenated and carbon dioxide-rich blood at the pulmonary capillaries. Simultaneously, the carbon dioxide waste is transferred from the deoxygenated blood into the lungs to be exhaled.
The now oxygen-rich and carbon dioxide-depleted blood travels from the pulmonary capillaries through the pulmonary veins and into the left atrium of the heart, where it transits to the left ventricle and systemic circulation.
SURFACTANT: Alveoli are aided by a thin film called surfactant made up of lipids and proteins, which cover their surface and prevent them from collapsing upon exhalation; they reduce the surface tension, thus preventing the lungs from sticking together or collapsing. (The surfactant hasn't yet been produced in very premature babies, causing severe respiratory compromise.)
Pulmonary Function Terms/Definitions
The lungs' ability to move air is far more complicated than it initially appears. Many interacting forces work together to keep the lung volume closely regulated. Several complex terms and definitions have been included below for completeness. The most important are tidal volume, minute respiratory volume, and lung compliance.
TIDAL VOLUME: the air that enters the lungs during a normal resting breath. The average tidal volume is approximately 500 ml in adults. The same amount of air leaves the lungs during resting exhalation.
MINUTE RESPIRATORY VOLUME: (Tidal volume x Respiratory Rate) Defines the volume of air that either enters or exits the lungs per minute.
VITAL CAPACITY: the maximum amount of air that can be moved by the lungs in one breath cycle. i.e., when you breathe out as much as possible, followed by taking the largest breath possible.
RESERVE VOLUME: accounts for physiologic dead space in the lungs. Reserve volume cannot be exhaled. This volume is the amount of air in the lungs after a maximal exhalation. This air reserve keeps the alveoli from collapsing.
LUNG COMPLIANCE: Lung compliance is defined as the ability of the lungs to stretch in response to movement of the diaphragm and chest wall. Low compliance is generally only seen in smokers and patients with severe lung diseases that slowly damage the tissue.