Quick and Dirty Guide to Childbirth I
Category: Special Populations
Topic: Obstetrics
Level: EMR
Next Unit: Quick and Dirty Guide to Childbirth II: The Delivery
10 minute read
The Quick and Dirty Guide to Childbirth I

Calls to EMS for OB emergencies especially, those where the patient is full term and in possible labor, are some of the scariest but, rewarding calls we face as medical professionals. It is important to have a thorough understanding of the development of the fetus as well as, emergencies that may arise for the newborn infant and/or mother during the pregnancy and delivery. In Childbirth I and II, we will concentrate on a normal delivery.
In the Beginning
There are many different "definitions" for when life begins:
- At conception, at which time a sperm encounters a fertilized egg and merges its genetic component with it, creating a unique, new version of the combined contributions from the mother (female, egg) and father (male, sperm).
- At implantation, when a fertilized egg has actually attached to the inner lining of the mother's womb (her uterus).
When a normal pregnancy begins; during ovulation the female ovary releases an ovum (egg) and begins its journey through the uterine tube. While in the uterine tube, sperm from the male, fertilizes the ovum to form a single-celled zygote. After a few days of rapid cell division, a ball of cells called a morula forms. The murola forms a hollow ball of cells called a blastocyte and implantation occurs, fetal development begins immediately. The normal duration of pregnancy is 40 weeks from the first day of the patient's last cycle.
Pregnancy is often described in trimesters, with each trimester lasting 13 weeks, or three calendar months.
- The first trimester is comprised of months 1 - 3, or weeks 1–15
- The second trimester consists of months 4 - 6, or weeks 16–27
- The third trimester includes months 7 - 9, or weeks 28–40
As Time Marches On
Placenta
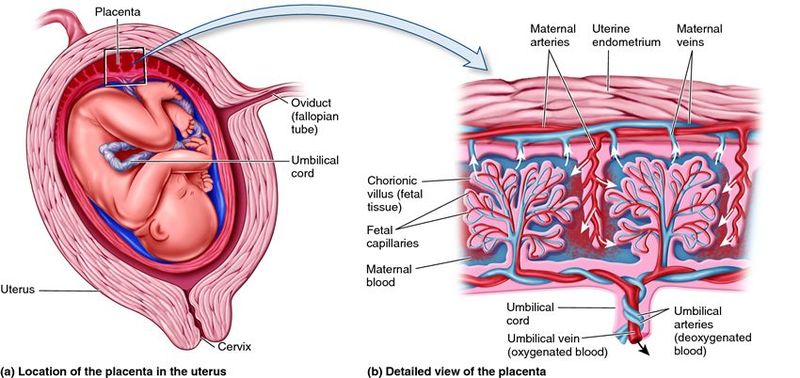
The placenta is formed about fourteen days after ovulation, it is a disc-like organ composed of interlocking fetal and maternal tissues, it is the organ of nutrient exchange between the mother and the fetus. The placenta is crucial for fetal development and is responsible for the following:
1. Transfer of gases: The diffusion of oxygen and carbon dioxide through the placental membrane and is similar to the same diffusion that occurs in the lungs. Dissolved O2 in the maternal blood diffuses into the fetal circulation. The carbon dioxide then diffuses from the fetal blood back into the maternal blood.
2.Transfer of nutrients: The other metabolic substances that the fetus needs, diffuse into fetal blood in the same manner as O2. The placenta also actively absorbs some nutrients from the maternal circulation. These substances include:
- Glucose
- Fatty acids
- Potassium
- Sodium
- Chloride
3. Excretion of waste: Waste products diffuse from fetal to maternal circulation and are excreted with the mother's waste. These waste products are:
- urea
- uric acid
- creatinine
4. Hormone Production: The placenta becomes a temporary endocrine gland by secreting estrogen and progesterone. This helps prepare the mother's body and the fetus for delivery.
5. Formation of a Barrier: The placenta forms a barrier from harmful substances and chemicals in the mother's circulation. The placenta is selective and only protects the fetus from some harmful substances, others can cross the barrier easily.
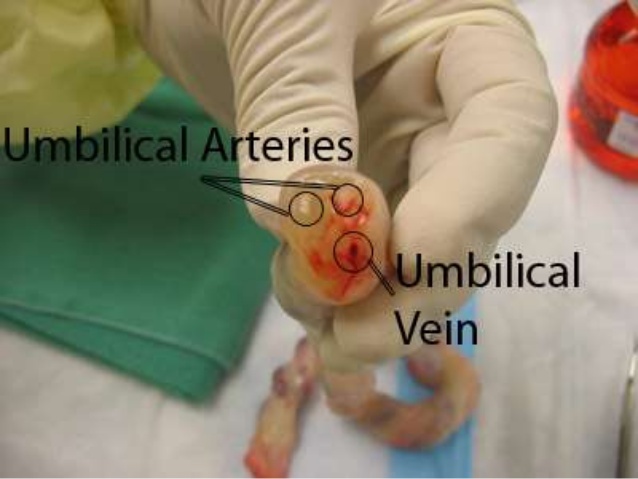
Umbilical Cord
The umbilical cord connecting the placenta to the fetus consists of one umbilical vein and two arteries and is present from the sixth week of pregnancy through delivery. The vein carries oxygenated blood toward the fetus; the arteries return the blood from the fetus to the mother.
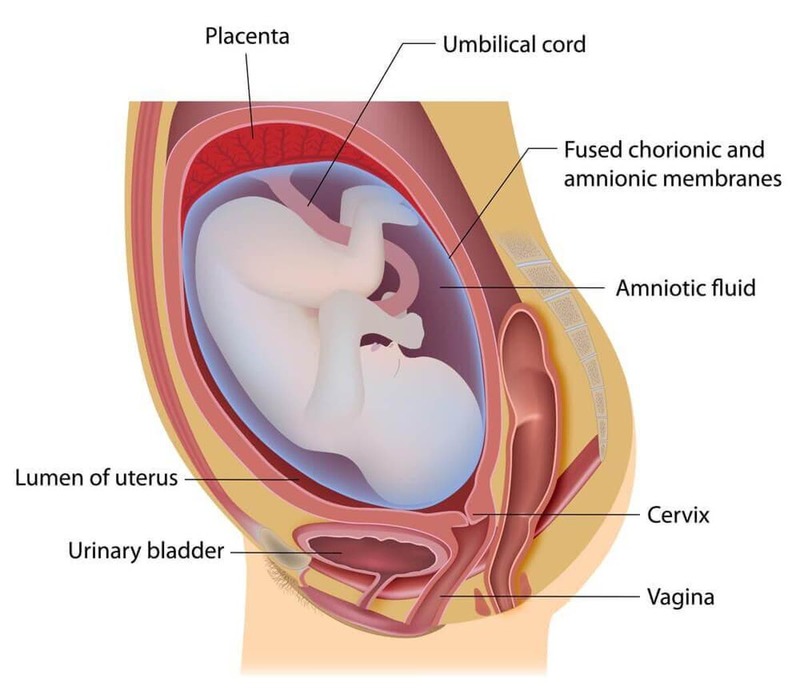
Amniotic Sac
While the placenta provides nutrients to the fetus and assists with the removal of wastes, the amniotic sac, which consists of membranes that cover the fetus, provides protection. The amniotic sac fills with amniotic fluid that is designed to protect the fetus and to provide an environment that is optimal for fetal development. A volume of up to one liter of amniotic fluid is maintained by the fetus's excretion of urine, as well as its swallowing of the amniotic fluid.