Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Pediatric SVT vs Sinus Tachycardia
Category: Special Populations
Topic: Pediatrics
Level: Paramedic
Next Unit: Pediatric Anatomy and Physiology
12 minute read
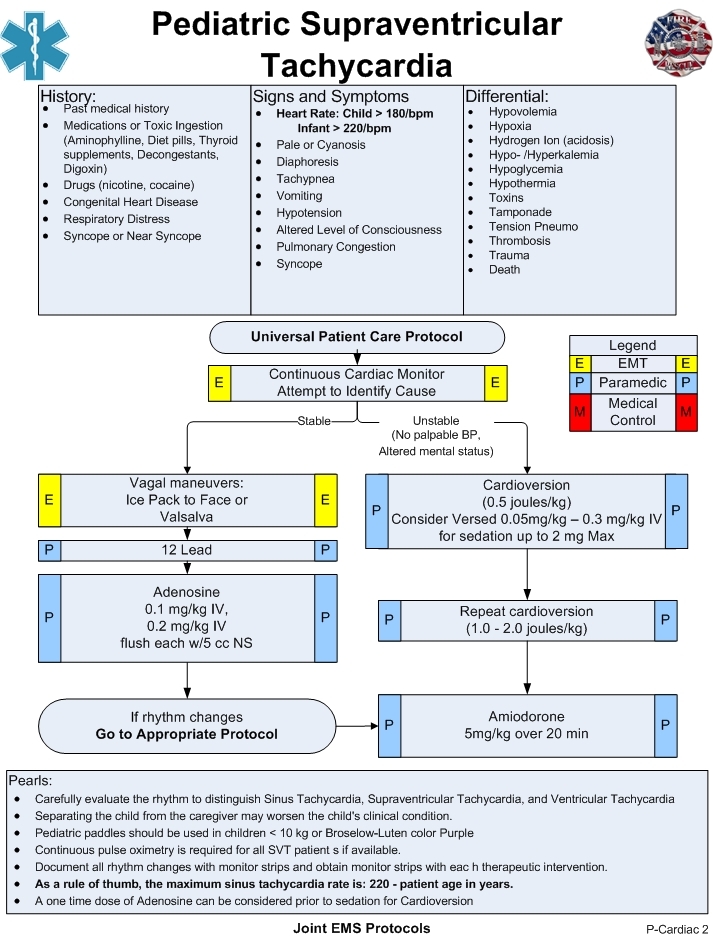
Pediatric SVT vs Sinus Tachycardia
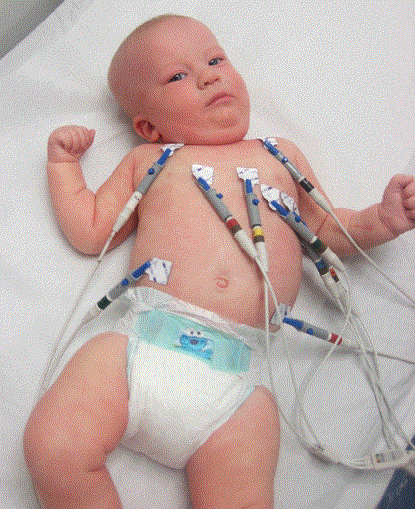
Believe it or Not!
Supraventricular tachycardia (SVT) is a common non-arrest dysrhythmia seen in children, especially during infancy, and is the main cause of cardiac-related instability. Most infants with SVT will outgrow the syndrome without lasting effects. History of the complaint is the key to proper distinction between SVT and rapid sinus tachycardia. The onset of SVT will usually show up in a normal child that is suddenly deteriorating with no history of a recent illness or injury. However, it must be carefully evaluated to ensure that proper treatment is implemented.
You do not want to cardiovert or administer adenosine to a child that is experiencing a fast sinus tachycardia and not SVT. Was the child sick? Think Sinus Tach! The best treatment modality will be aimed at discovering and correcting the underlying cause.
Don't forget the H & T's!
SVT v/s Sinus Tach in Pediatrics
1. Patient History: The history of events leading up to calling for EMS assistance can offer valuable information in choosing the correct treatment modality for the child:
(SAMPLE format works well when acquiring a pertinent history)
- Has the child been ill?
- Is he dehydrated?
- Is there bleeding that may be associated with shock?
- Does he have any known medical problems?
- Has this happened before and if so, what was done then to correct it?
- Does the child have any known drug allergies?
2. Heart rate: Sustained heart rate during the event
(Check out the Q & D Guide to Pediatric Assessment for an awesome vitals chart and other useful pedi-info)
- Infant: Sinus tachycardia is usually < 220 bpm; Supraventricular tachycardia is usually > 220 bpm
- Child: Sinus tachycardia is usually < 180 bpm; Supraventricular tachycardia is usually > 180 bpm
EKG Findings
Important EKG findings in pediatric sinus tachycardia:
- Heart rate will be < 220 bpm in an infant and < 180 bpm in children
- Variable R-R waves
- P waves present and upright in leads II, III, aVF
Sinus Tachycardia is normally secondary to:
- Dehydration
- Hypovolemia (most common)
- Fever
- Hypoxia
- Anemia
- Shocks
Sinus Tach is not that uncommon in children but is normally caused by a contributing factor and not a true cardiac cause
Important EKG findings in pediatric supraventricular tachycardia:
- Heart rate will be > 220 bpm in infants and > 180 bpm in children
- Non-variable R-R waves
- The rhythm will be consistently regular (because associated AV block is extremely rare in infants/children)
- The P waves may be non-identifiable, especially when the ventricular rate is high
- If P waves are present, they will likely be inverted in leads II, III, and aVf
- QRS complex duration is 0.10 second in most cases
- SVT with QRS complex > 0.10 is extremely rare in infants and children
SVT seen in children may be of several types:
- Reentry with an accessory pathway (Wolf-Parkinson-White)
- Reentry without an accessory pathway
- Spontaneous depolarization of pacemaker sites
- Cardiac pathology (i.e: Ebstein's anomaly)
- Pharmacological influences: (medications containing sympathomimetic amines, caffeine)
- Metabolic influences: (endocrine abnormalities, hyperthyroidism, etc.)
Symptoms/Management of Pediatric SVT
Signs and symptoms during supraventricular tachycardia are affected by the child's age, duration of the SVT, prior ventricular function, and ventricular rate.
Infants with sustained episodes of SVT will present with:
- Tachypnea
- Loss of interest in feeding
- Irritability
- Progressing over 24-48 hours to lethargy
- Sternal and intercostal retractions
- Cardiovascular signs of a weak pulse, ashen color, etc.
If a child is hemodynamically stable and cooperative vagal maneuvers may be effective and are safest; such as:
- Ice water applied to the face
- Blowing through a straw
- Carotid sinus massage
IMPORTANT NOTE: An absolute contraindication to adenosine is sinus tachycardia (ST). Dehydrated patients, especially infants and young children with fever, failure to thrive, and/or an infection may appear to be in SVT, when in fact they’re barely compensated with a sinus tachycardia with a rate that may be greater than 180-200 bpm. Patients that are experiencing rapid sinus tachycardia are at high risk for morbidity and mortality if adenosine is administered. Contact medical command early!
"Treat the patient and not the monitor"
- Emergency pharmacological therapy consists of Adenosine
(0.1 mg/kg {max 1st dose 6 mg} by rapid bolus, may double 1st dose - 0.2 mg/kg {max 2nd dose 12 mg}) - Wolf-Parkinson-White (WPW) syndrome must be ruled out prior to treating as SVT
- Electrical emergency treatment includes Synchronized Cardioversion at 0.5 -1.0 joule/kg.
(Don’t forget to sedate prior to cardioversion when appropriate)