Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Infant Growth and Development (0-1)
Category: Medical
Topic: Life Span Development
Level: EMT
Next Unit: Toddlers and Preschool Age (1-5)
17 minute read
Infant (0 -1 year) Physiology
Vital signs
Normal heart rate in newborns is between 140 and 160 beats per minute. It often ranges between 100 and 160 beats per minute during the first 30 minutes of life and settles to around 120 beats per minute after that. However, a normal resting heart rate can range from 80 to 160 beats per minute in infants 1 to 11 months of age.
Normal respiratory rate in newborns is between 40 and 60 and drops to 30-40 after the first few minutes of life. Respirations slow to 20-30 breaths per minute by one year of age.
Normal tidal volume at birth can be approximately 15 milliliters, with increases expected to be approximately 120 to 180 milliliters for a 1-year-old. But what is required, according to the formula used with newborns, is
4-6 ml/kg. Some sources indicate 6-8ml/kg, but for lung protective strategy for newborns, 4-6ml/kg is recommended.
(a 3.4 kg baby would require a tidal volume not to exceed 20.6 ml.)
When the infant turns 1 year old, the formula goes to 6-10 ml/kg.
Sleep: Newborns sleep about 16-18 hours a day, total, split between daytime and nighttime, including waking up every few hours.
Average systolic blood pressure increases from 70 mmHg at birth to 90 mmHg at one year old.
Normal temperature ranges for this age group are between 98 to 100 degrees Fahrenheit.
Weight - Normal weight of 3.0-3.5 kg (6.6-7.7 lbs) at birth, with a normal decrease in birth weight of 5-10% in the first week of life. The infant's head is equal to 25% of the total body weight.
Pulmonary system
Airways are shorter, narrower, less stable, and more easily obstructed as infants, who are primarily nose breathers until 4 weeks old. Lung tissue is fragile and prone to trauma from pressure. Fewer alveoli are present with decreased collateral ventilation. Accessory muscles are immature and susceptible to early fatigue. The chest wall is also less rigid. Diaphragmatic breathing may be present. Rapid respiratory rates lead to rapid heat and fluid loss.
Immune system
Newborns and infants have what is known as passive immunity retained through the first six months of life, which is based on maternal antibodies received from their mother. After the first six months of life, this immunity begins to fade, and the risk of vaccine-preventable illnesses rises significantly.
Nervous system
Infants have strong, coordinated suck and gag reflexes, well-flexed extremities, and move extremities equally when the infant is stimulated.
Reflexes
Infants and newborns have inherent reflexes known as the rooting reflex, the suck reflex, the Moro reflex, the tonic neck reflex, the grasp reflex, the Babinski reflex, and the stepping reflex. 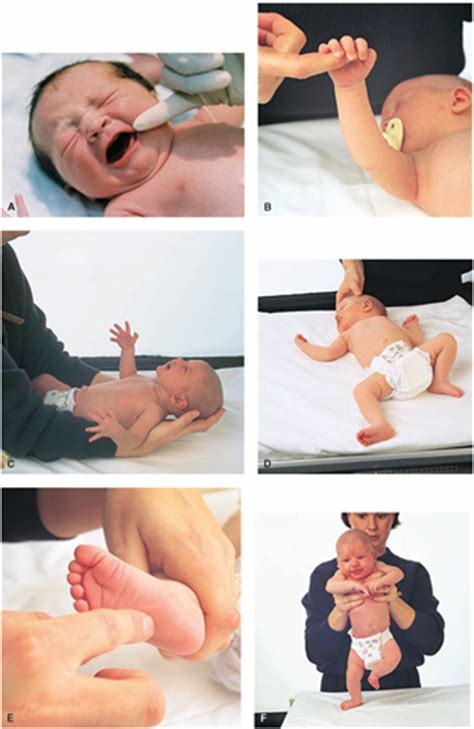
- ROOTING REFLEX: when the baby turns his or her head toward any stroke or touch of the corner of their mouth, helping the baby to find the breast or bottle.
- SUCK REFLEX: follows the rooting reflex, and occurs upon touching the roof of the baby’s mouth.
- MORO REFLEX ("startle reflex"): when the baby throws back their head, extends their arms and legs, cries, then pull the arms and legs back in as a response to loud stimuli or movement.
- TONIC NECK REFLEX: when the baby’s arm stretches out on the same side that the neck is turned to, as well as the opposite arm bending at the elbow.
- GRASP REFLEX: when the baby’s fingers close upon stroking of their palm.
- BABINSKI REFLEX: when the big toe bends back toward the top of the foot and the other toes fan out on the foot that has been firmly stroked on the lateral sole of the foot.
- STEP REFLEX: when the baby appears to take steps or dance when held upright with their feet touching a solid surface.
Note: as the infant's nervous system matures, nerve development that suppresses these infant reflexes begin to dominate at 6 months, and these reflexes go away. This is significant in a neurological exam of an elderly patient because re-emergence of these reflexes indicates brain damage to these suppressive areas.
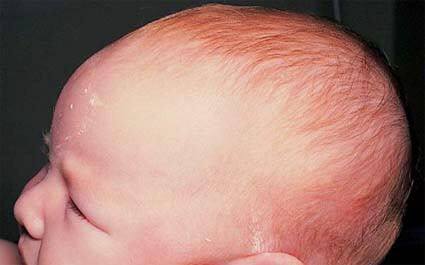
Fontanelles
Newborn and infant skulls are not completely closed, with openings known as the fontanelles. The posterior fontanelle closes at three months and the anterior fontanelle closes between 9 and 18 months. An assessment of the fontanelles (bulging = increased pressure sunken = dehydration) may provide an indirect estimate of hydration status of a newborn or infant. This is common while an infant is crying, vomiting, or lying down; if they are truly bulging while the infant is calm and upright, this indicates increased cranial pressure; possible causes include encephalitis, hydrocephalus, or meningitis.
Growth and Development in Infants:
- Newborns undergo rapid changes over the first year of life.
- At two months old, the baby begins tracking objects with their eyes and recognizes familiar faces.
- At four to five months old, a baby begins to develop "Object Permanence," a general understanding that objects continue to exist after they leave the child's line of sight. This is the beginning of separation anxiety in most infants, as they know that crying or cooing will result in a caregiver returning.
- At six months old, a baby will sit upright without back support and make one-syllable sounds (for example, “ma,” “da,” etc).
- At 12 months old, a baby will walk with assistance. Some may begin walking unassisted and should know their own name. This varies greatly from 9 months-18 months of age.
Sensorimotor Development
20th Century psychologist Jean Piaget broke down the sensorimotor stage of development into 6 stages:
- Birth to 1 Month: Reflexes: the main way infants relate to the world, i.e., rooting, sucking, and startling.
- 1-4 Months: Grouping of interactions and experiences, e.g., realizing sucking his/her thumb is placating, so repeating.
- 4-8 Months: Intentional actions to create a response.
- 8-12 Months: Exploration, e.g., shaking a toy to see it move or make a sound. Will begin walking with assistance.
- 12 to 18 Months: Trial-and-error: experimentation. Will begin walking unassisted.
- 18-24 Months: Object Permanence continues, which began at about four months: when objects continue to exist even without being seen or felt. They can symbolically imagine things. This can happen in some infants by 8-9 months.
Psychosocial Development
Newborns and infants develop differences in cries, including
- basic crying (systematic cry with a repetitive pattern of crying and silence),
- hunger crying (rhythmic, with steady wavelike variations in volume and urgency),
- anger crying (like the basic cry, but with more excess air forced through the vocal cords, making it louder and more abrupt),
- pain crying (generally sudden--no preliminary moaning or build-up, begins with an inward gasp, and results in a loud rising shriek).
They also exhibit a response to situational crises, such as parental separation, with protest, despair, and withdrawal.