Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Common Neurological Conditions
Common Neurological Conditions
This section will review some of the neurological conditions commonly encountered by critical care and flight paramedics.
Cerebrovascular Accident (Stroke)
Cerebrovascular Accident (Stroke)
A cerebrovascular accident (CVA), or stroke, refers to the loss of blood flow to a section of the brain due to damage to or blockage of the blood vessels. Patients with CVAs almost always present with some form of neurological finding and can have severe systemic complications.
There are three types of CVAs:
-
Thrombotic Stroke: The most common form of ischemic stroke, caused by a blood clot forming directly in an artery supplying the brain. This type of stroke is often associated with atherosclerosis and accounts for the majority of ischemic strokes.
-
Embolic Stroke: A less common form of ischemic stroke, occurring when a blood clot travels to the brain from another location in the body. Atrial fibrillation is a common cause of embolic strokes.
-
Hemorrhagic Stroke: A less common form of stroke overall, occurring when a small vessel or aneurysm ruptures. The spilled blood within the brain damages neurons directly, and the loss of blood flow also leads to ischemic damage.
Air medical treatment
Assuming a patient's ABCs are initially stable, assessing disability is vital. This gives the receiving facility an indication of what level of treatment is likely to be required.
- Ensure that the time of the patient's last known normal is known. This is vital to determining what treatment to provide in the hospital setting. Patients that could have had more than 4-12 hours since their CVA began are generally given less aggressive treatments due to the low chance of serious recovery.
- The National Institutes of Health Stroke Scale (NIHSS) is a tool used to formally assess the amount of disability from a stroke and guide treatment. The use of this tool in transport will depend on your local jurisdiction.
The in-transport treatment of any CVA is focused on maximizing blood flow to the brain, minimizing intracranial pressure elevations, and managing any complications that place the airway at further risk.
- Airway: Assess neurological status regularly and intubate if early signs of elevated ICP develop, the GCS drops below 9, or the patient is rapidly declining.
- Breathing: Consider permissive hypercapnia in the intubated patient. Otherwise, watch for respiratory depression due to elevating ICP or decreasing mental status.
- Circulation: Keeping the blood pressure close to the patients normal is vital. Excessively high blood pressure can lead to increased damage in hemorrhagic strokes. Low blood pressure will increase the amount of brain tissue damaged in any form of stroke.
Skull Fractures
Most skull fractures are rarely serious on their own but suggest that severe injury to the brain may also be present.
- Linear Fracture: A simple line-like fracture extending towards the base of the skull.
- Linear Stellate Fracture: Multiple linear fractures that radiate from the point of impact.
- Diastatic Fracture: Separation of skull bones at an anatomic suture line.
- Depressed Fracture: A compressed area on the surface of the skull.
- Basilar Fracture: A fracture at the base of the skull. These fractures can lead to meningitis, damage to cerebral blood vessels, and damage to cranial nerves. Numerous signs point to a potential basilar fracture.
- Battle's sign: Bruising behind the ears.
- Periorbital ecchymosis: especially around the medial aspect of the eye sockets.
- Otorrhea: Leakage of CSF from the ear.
- Rhinorrhea: Leakage of CSF from the nose.
Impacts strong enough to result in skull fractures lead to many potentially fatal complications that are reviewed in other sections. Intracranial bleeding, seizures, and cerebral edema leading to severe elevations in ICP are all very common. Patients could be transferred from a scene prior to stabilization requiring aggressive ICP reducing interventions or may decompensate while in transit between a smaller and specialty facility. Meningitis, encephalitis, and damage to cranial nerves and blood vessels may occur days to weeks after injury and could result in an inter-facility transfer by critical care ambulance.
Maxillo-Facial Injuries
Facial fractures are closely related to skull fractures. The trauma that leads to one can easily cause the other. The same complications as skull fractures exist. Facial injuries also risk airway compromise due to swelling in and around the oropharynx.
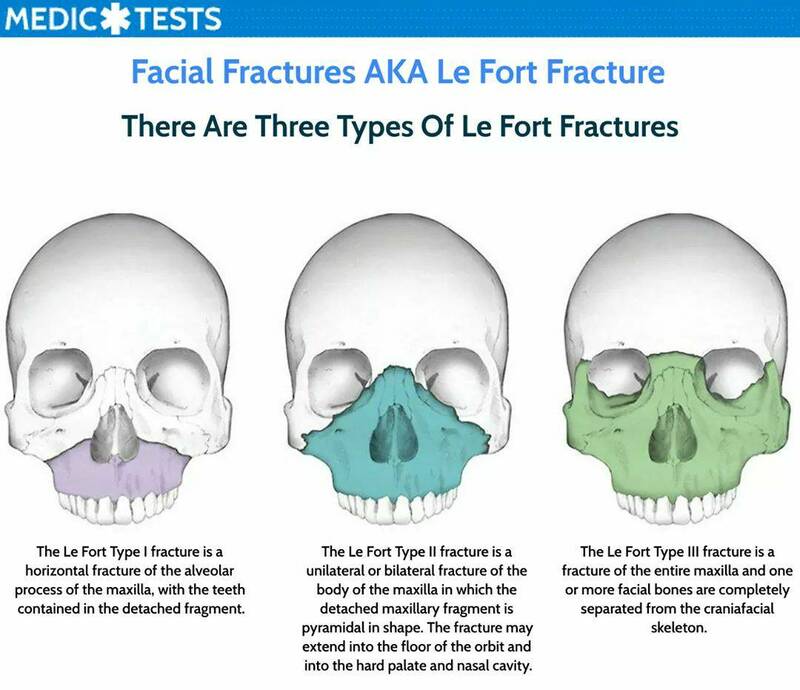
Facial fractures are classified by "LeFort categories." These fractures can lead to a sensation of facial "mobility" with palpation and diffuse bruising over the face. All LeFort fractures are a contraindication to airway access via the nose, and all have a significant risk of airway compromise.
- LeFort I: Fracture of the bilateral upper maxilla.
- LeFort II: Fracture of the bilateral midface beneath the orbits.
- LeFort III: Fracture of the bilateral midface through the orbits and with a full separation of the facial bones from the skull.
Consider early intubation for patients with severe LeFort fractures and close monitoring for any patient with facial trauma.
Spinal Cord Syndromes
Three primary spinal cord syndromes are seen in the air medical setting; all are managed with conservative measures.
- Brown-Sequard: Disruption of one half of the spinal cord while the other half remains intact.
- Very rare and generally only occurs with penetrating injury, but appears on exams often as it illustrates neuroanatomy.
- Ipsilateral loss of motor control (no motor movement of
- Contralateral loss of pain and temperature sensation:
- Central Cord: Disruption of the center of the spinal cord while the edges remain intact.
- Most commonly occurs due to forced extension or flexion of the neck, commonly in car accidents.
- Results in greater weakness and abnormal sensation in the upper extremities as opposed to the lower extremities.
- Anterior Cord: Disruption of the anterior portions of the spinal cord.
- It generally occurs due to aortic dissection or surgery as the vessel that feeds the anterior spinal cord comes directly off the aorta.
- Touch and proprioception (sense of position) are maintained, but movement, pain, and temperature sensation are lost beneath the lesion.
Complications of spinal cord syndromes
There are two main complications of spinal cord injury that can lead to an acute change in patient status neurogenic shock and autonomic dyslexia.
Neurogenic shock tends to occur acutely right after the injury. Loss of sympathetic innervation below the injury leads to vasodilation and resulting hypotension. Neurogenic shock can occur any time after injury.
- Hypotension, warm/red skin, and the absence of compensatory tachycardia are the most common signs.
- Manage like any other distributive shock: IV fluids and pressors are the mainstays of treatment.
- Phenylephrine and epinephrine are excellent for neurogenic shock. They activate alpha receptors, which cause the blood vessels to constrict, replacing the loss of the sympathetic nervous system.
Autonomic dysreflexia tends to occur in patients living with spinal cord injury for several weeks to months. The presence of a noxious stimulus (such as a full bladder or skin injury) that the patient cannot physically feel due to sensory nerve disruption leads to a dramatic sympathetic response.
- Can result in hypertensive emergency and resulting myocardial infarction, CVA, retinal hemorrhage, or seizure.
- Treat by removing the offending stimuli if able. It can be as minor as uncomfortable positioning on a spinal board or a small object beneath the patient.
- Control hypertension with nitro-based medications, ensure that the patient's bladder is empty, and treat any complications as they arise.
Coma
A coma is a state of deep unconsciousness that lasts for a prolonged period of time. Rarely patients in a true coma may be transported by critical care services between hospitals. More commonly, a patient will have a low Glasgow coma score that does not improve with any intervention. These patients are often referred to as "comatose," but the correct technical term in the EMS setting is "persistently unresponsive."
Etiology
Any medical condition or injury that leads to damage or dysfunction of the cells in the central nervous system can lead to a coma. Some of the most common causes encountered in the critical care and air medical setting are reviewed here:
- Hypoglycemia or hyperglycemia
- Overdoses of any drug (including alcohol)
- Seizures
- Hypoxia
- Psychiatric illness
- Ongoing or previous CVA
- Increased intracranial pressure
- Sepsis
- Uremia (due to hepatic or renal failure)
- Shock of any etiology
Treatment
In transport, managing an unconscious or unresponsive patient is focused on monitoring and securing the ABCs. The airway and breathing are always compromised in these patients, and intubation is universally required if the altered state cannot be quickly reversed.
In the persistently unresponsive patient:
- Monitor ventilation and ensure no acute changes occur due to altitude changes or failure of the endotracheal tube/tracheostomy.
- Maintain spinal immobilization in patients suspected of having a spinal injury.
In the acutely unresponsive patient:
- Quickly assess the ABCs
- Attempt the following interventions if indicated to acutely restore consciousness
- Narcan: If opioid overdose is suspected
- Dextrose: If hypoglycemia is suspected
- Thiamine and dextrose: if chronic alcohol use is suspected
- Consider intubation if the above does not restore consciousness
Diagnostics
Acutely unconscious patients will generally get the following diagnostic tests done before transfer to another facility. Post intubation blood gasses and X-Rays should be obtained.
- CT scan of the head
- CBC and blood chemistry panel
- Urinalysis and urine drug screen
- Arterial blood gas (as needed to monitor effects of ventilator changes)
Epilepsy and Seizures
Seizures leading to critical care transport or transfer are commonly due to severe neurological injury or an underlying seizure disorder. The treatment of seizures in the critical care setting is heavily skewed towards the treatment of status epileptics.
The typical presentation of a seizure follows a predictable pattern:
- Aura: An abnormal visual, olfactory, or physical sensation that typically precedes the patient's seizures. These are often only recognized by patients with severe recurrent episodes.
- Tonic: An initial period of muscle stiffening throughout the body.
- Clonic: The classic convulsion that typifies a general seizure in most individuals, a rhythmic contraction and loosening of the muscles in the body.
- Postictal: A period of confusion, memory loss, and altered mental status that follows the cessation of clonic activity.
Treatment
The treatment of the acute seizure episode is focused on supporting and protecting the patient while attempting to terminate seizure activity. All seizures are treated similarly regardless of their etiology. If there is a known underlying etiology, treating that is the best way to prevent recurrent seizures.
- Monitor the airway and breathing closely. Patients may aspirate during a seizure or have a prolonged postictal state that places them at risk for aspiration. Consider intubation in patients with recurrent or continuing seizures despite giving the medications below.
- Place padding around any patient with a seizure to prevent secondary injuries from the clonic phase if seizures recur.
- Immediately terminating seizure activity in transit is generally appropriate as a restrained patient in a confined space that is supine has a high risk for further injury. The following medications are classicly used for seizure termination.
- Benzodiazepines
- Lorazepam (ativan) IV or IM 4–8 mg
- Diazepam (valium) IV or IM 5–10 mg
- Phenytoin (dilantin) IV 15–20 mg/kg
- Barbituates
- Phenobarbitol IV 15–20 mg/kg
- Considered a third-line agent due to respiratory depression and aspiration risk.
- Intubation and sedation medications
- Propofol sedation is most commonly used
- Any paralytic agent can be chosen
- Benzodiazepines
- If there is a suspected etiology of the seizures correcting that abnormality is the best way to prevent a recurrence. Some of the most common etiologies are:
- Hypoxia
- Hypoglycemia
- Discontinuation of anti-epileptic medications
- Sepsis/Meningitis
- Status epilepticus is the presence of more than five minutes of seizure activity or the presence of a second seizure in the postictal period. If this occurs, treat aggressively, status epilepticus is associated with very poor outcomes if untreated.
Guillain-Barre Syndrome (GBS)
GBS results from the death of the myelin cells that surround the axons in the peripheral nerves. It commonly occurs after an acute infectious illness or several days following the administration of certain drugs. It is suspected to be the result of an autoimmune process.
Signs and Symptoms
GBS almost always presents as a weakness that begins in the lower limbs and progresses towards the trunk. This is known as "ascending" paralysis.
- Deep tendon reflexes generally disappear in paralyzed areas.
- Women are affected 5x more often than men.
- An acute diarrheal illness or nonspecific viral illness usually occurs several days before symptoms develop.
- Patients with paralysis ascending into the trunk generally begin to exhibit signs of gradual respiratory failure.
Treatment
Patients that do not have respiratory involvement rarely require any emergency measures. These patients rarely end up in critical care or air medical ambulances. Those with severe respiratory involvement should be intubated and sedated prior to transport. Altitude and the reduction in the patient pressure of oxygen combined with having to lie flat can lead to respiratory failure in a slowly decompensating GBS patient. Attention to the airway and breathing is the only specialized care required for GBS patients.
Myasthenia Gravis (MG)
MG is the rapid fatigue of muscles in the body due to the blockade of the acetylcholine receptors in the neuromuscular junctions. This blockage occurs due to the creation of antibodies against these receptors by the body.
Signs and Symptoms
Weakness, fatigue, and exercise intolerance are the primary signs of MG.
- Fatigue of the small muscles in the eyes and eyelids presents first. This leads to ptosis and double vision.
- Patients may lose control of the head and neck and small muscles of the hands.
Myasthenic crisis is the presence of a severe exacerbation of this weakness that begins to affect the diaphragm and other chest wall muscles. This leads to potentially rapid respiratory failure.
Treatment
MG patients undergoing critical care transport are generally in a myasthenic crisis. They should be intubated and sedated prior to transport, as respiratory failure will be exacerbated by supine positioning and altitude.
- Monitor the patient's airway and respirations closely.
- Patients may be placed on BiPAP if not initially intubated.
- Unless the patient is intubated, do not use atropine at any time.
- Avoid succinylcholine for intubation, as it can lead to prolonged paralysis.
Acute Meningitis
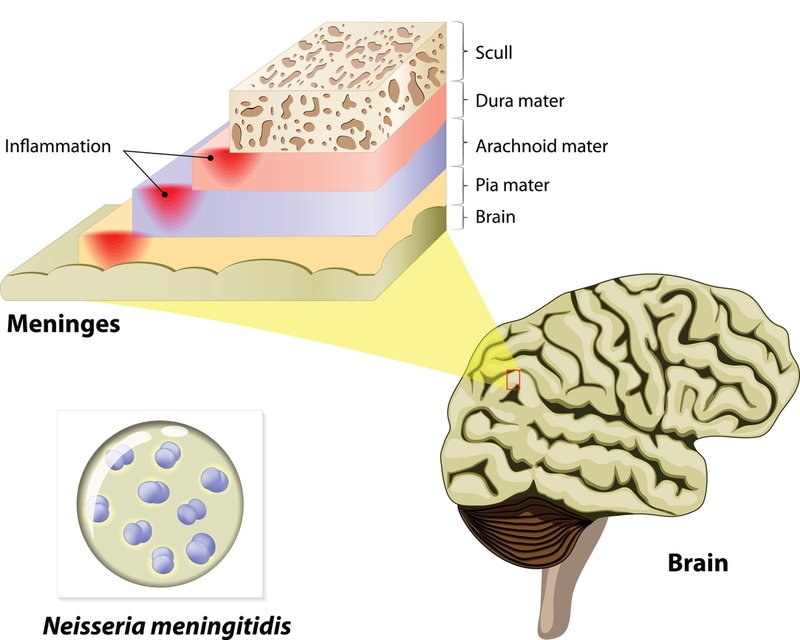
Meningitis is inflammation within and around the brain's lining. Bacterial infection is the most common cause of severe acute meningitis, which can lead to critical care transport. Viral infections, fungal infections, and autoimmune syndromes are less common but still dangerous causes of meningitis.
Signs and Symptoms
Meningitis progresses rapidly and has very specific signs and symptoms in many patients, unlike many conditions.
- Fever, chills, fatigue, and altered mental status are common symptoms.
- Headache, photophobia, vomiting, and pain when turning the neck are common as meningitis progresses.
- The inability to turn the neck and extend or flex the neck is known as "meningismus" and is a warning sign of severe illness.
- Kernig sign: Pain in the lower back and neck when the leg is extended at the hip and knee.
- Brudzinski sign: Flexion of the hips and knees in response to forced flexion of the patient's neck.
Treatment
Treating meningitis is focused on initiating antibiotics, antivirals, or antifungals early. Monitoring for and treating complications of infection takes precedence in transport and early in the patient's hospital course. Often, these patients will be stabilized and transferred after antibiotics and other anti-infectives have been initiated.
- Place the patient in droplet precautions. Some types of bacterial meningitis are highly contagious.
- Monitor for acute changes in the ABCs. A patient's mental status may rapidly decline and compromise their airway and breathing. They may also develop sepsis that can lead to rapid hypotension.
- Treat mental status decline with early intubation.
- Sepsis should be treated with IV fluids, dexamethasone, and antibiotics, all of which should be continued in transit.
- Elevations in ICP may result from acute damage to brain tissue or obstruction in the normal flow patterns of CSF from bacterial breakdown products.
- Manage ICP like brain bleeds: elevating the head of the bed, permissive hypercapnia, mannitol, and paralytic/sedative agents.
- A lumbar puncture should be performed at the referring facility to target antibiotic agents and determine the type of meningitis the patient presents with.
- A CT scan is also often done at the referring facility to rule out subarachnoid hemorrhage as a cause of meningeal signs.
Encephalitis
Encephalitis is inflammation of the brain tissue itself and often results from meningitis. Viral meningitis due to herpes or varicella-zoster generally leads to the most severe forms of encephalitis.
Signs and Symptoms
Encephalitis generally presents with the signs and symptoms of meningitis listed above. In the rare case of encephalitis existing without meningitis, symptoms may not include the signs of meningeal irritation, such as neck rigidity, the Kernig sign, and the Brudzinski sign.
Treatment
Managing a patient with encephalitis is nearly identical to managing meningitis. These patients will typically be intubated and sedated due to the extreme risk of rapid decompensation.
Severe elevations in ICP are more common in patients with both encephalitis and meningitis than in patients with a single condition.