Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Chest Trauma Overview
Category: Trauma
Topic: Chest Trauma
Level: EMT
Next Unit: High Yield Thoracic Injuries
10 minute read

Chest trauma is one of the most common causes of death in trauma, accounting for 25-50% of all trauma-related deaths.
Chest trauma can roughly be divided into
- BLUNT (e.g., steering wheel) and
- PENETRATING (e.g., knife) causes,
with some significant overlap.
ENERGY IMPACT: The "energy" of the injury is also vital to consider:
- LOW-ENERGY INJURIES: tend to be localized to the immediate area that was impacted/impaled.
- HIGH-ENERGY INJURIES: can result in a multiple-trauma or "polytrauma" situation, which is significantly more dangerous for the patient.
The amount of energy applied to objects in motion and the way they impact the body dictates the extent of the injury. The most common situations leading to chest trauma are as follows...
- Automobile accidents.
- Falls from excessive heights (usually over 10 feet).
- Blast injuries (explosives or pressurized air/water).
- Significant blows to the chest.
- Crush injuries.
- Gunshot wounds (GSW).
- Stab/impalement wounds.
While some of these seem obviously penetrating or blunt, each can have varying presentations and severity.
A small car accident could result in no trauma, while a major one may result in blunt and penetrating injuries. Likewise, a gunshot into a kevlar vest may result in no penetration, yet have life-threatening blunt injuries. This is an area where a thorough patient assessment is vital.
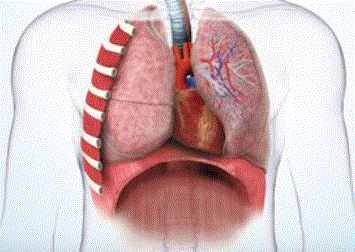
Tissue Involvement in Chest Trauma
Beyond the mechanism of injury, identifying the tissues involved in trauma is vital. There is potential for injury to the
- Skeletal
- Pulmonary
- Vascular
- Cardiac systems.
SKELETAL:
The ribcage is vital to the expansion of the lungs; if enough ribs are damaged the chest will be unable to expand in response to movement of the diaphragm, leading to inadequate ventilation and resulting in injury or death. Also, the pain of expanding the chest against damaged ribs can cause a patient to splint the pain by voluntarily limiting the diaphragm movement.
These injuries can present in many ways. A single rib fracture may cause patients enough pain to reduce breathing appreciably, while others may have severe sternal fractures or multiple damaged ribs, leading to "flail-chest" which is discussed in detail later.
PULMONARY:
The 3 major structures of the pulmonary system can be directly damaged by trauma:
- Lungs
- Bronchi
- Trachea
- Acutely, a crushed trachea or severed bronchus will lead to severe airway compromise.
- Sub-acutely, bruising of the lung can lead to decreased oxygen saturation and may be fatal in even otherwise healthy patients.
- The possibility of hemothorax and pneumothorax in blunt or penetrating trauma may also compromise breathing.
VASCULAR:
While rarer than other causes, damage to the "great vessels" that carry blood to and from the heart and lungs can lead to extremely rapid death, due to the massive volume of blood these vessels carry.
- Injury to these vessels is associated with instant death in high-energy blunt trauma events, but
- minor injury from penetrating trauma or lower energy blunt trauma may lead to a patient's slow decline during transport.
CARDIAC:
The heart itself is extremely vulnerable without the protection of the skeleton.
- Direct bruising of the heart is usually fatal.
- Any impact on or near the heart can lead to arrhythmia, including "minor impacts." [DISCUSSED LATER]
- Penetrating trauma to the heart can lead to rapid death from exsanguination or cardiac tamponade and resultant hypotension.
- And finally, any case of severe blood loss can result in the heart losing the ability to pump blood correctly [DISCUSSED IN THE SECTION ON SHOCK].
Management
Management of these systems in acute trauma focuses on identifying what is damaged and applying the relevant lifesaving measure.
At the EMR/EMT/AEMT level, rapid recognition of these conditions via an expert-level primary survey is key.
- The ABCs will often identify the presence of a major injury.
- A more detailed exam will identify the system responsible.
- And regular reassessments of patient status and vital signs will give patients the best chance for survival in the pre-hospital setting where things can change very quickly.
[The details of assessment and management of chest injury will follow in future sections.]