Test Complete
- Questions
- Score
- Minutes
| Overall Results | |
|---|---|
| Total Questions |
| Category Results | |
|---|---|
Body Substance Isolation
Category: Medical
Topic: Infectious Diseases
Level: EMT
Next Unit: Exposures and Transport Decisions
12 minute read
Body Substance Isolation (BSI): The Basics and Beyond
BSI is an essential practice that protects both patients and healthcare providers from infectious diseases like HIV, hepatitis, and other contagious illnesses. By isolating all body substances (blood, urine, feces, tears, etc.), we significantly reduce the chances of disease transmission.
Why Body Substance Isolation?
BSI isn't just about donning gloves or washing hands; it's a comprehensive strategy formed with input from numerous agencies, including OSHA, Highway Safety, and the CDC. But why is it crucial in an EMS setting? Without proper BSI practices, you expose yourself and other patients to disease. You don't want to be at a random MVC where someone has an open cut, and the next thing you know, you're bringing home some communicable disease to share with your family. Bad things can still happen even when trying to do good in the world. Mitigate ALL possible risks and go home safe to live a long, healthy life at the end of the day.
Hands in the Field: More than Just Clean
Handwashing is the cornerstone of BSI. Our hands are our primary tools in the field. Thus, they are also the likely point of contact with infectious substances. Current guidelines recommend two methods for hand cleaning: using an alcohol-based hand sanitizer and washing with soap and water.
Guidelines suggest cleaning before eating, before and after having direct contact with a patient's intact skin (taking a pulse or blood pressure, performing a physical examination, lifting a patient in bed); after contact with blood, body fluids, or excretions, mucous membranes, non-intact skin, or wound dressings; after contact with inanimate objects (including medical treatment) near the patient; if hands move from a contaminated body site to a clean body site during patient care; after glove removal; and after using a restroom.
- The primary purpose of hand soap is to remove germs and bacteria, not kill them, and clean the hands. When washing your hands with soap, dirt, and germs trapped in the skin's natural oils are lifted and suspended in water.
- On the other hand, alcohol-based hand sanitizer is proven to kill viruses and bacteria, but this is limited if the hands are visibly soiled. The alcohol-based sanitizer has the negative consequence of killing healthy bacteria and degrading the quality of your skin flora.
Alcohol-based Hand Sanitizer
Alcohol-based hand sanitizer is used on dry hands by putting a quarter-sized amount of product in one palm and rubbing the hands together for approximately 20 seconds, covering all surfaces until hands feel dry,
Handwashing with Soap and Water
Washing hands with soap and water is performed by first wetting hands with warm water, then applying the amount of the soap product recommended by the manufacturer to the hands, and then rubbing hands together vigorously for at least 15-20 seconds, covering all surfaces of the hands and fingers, followed by rinsing hands with warm water and using disposable towels to dry and, finally, using disposable towels to turn off the faucet.
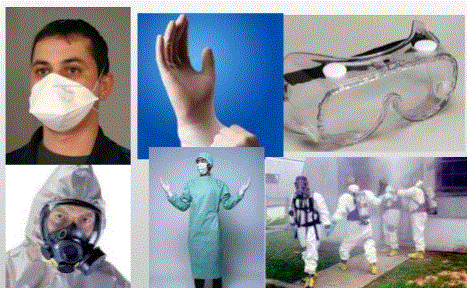
Armor Up: Personal Protective Equipment (PPE)
Think of PPE as your personal armor against invisible enemies. It's more than just gloves; it's about wearing the right level of protection for the situation.
Current recommendations for personal protective equipment (PPE) include:
- always wearing gloves and changing gloves when treating a new patient,
- wearing eye, clothing, and face protection during events where blood or other bodily fluids are expected, and
- wearing isolation masks--including N95 masks--when respiratory infectious diseases are expected or suspected.
PPE guidelines also include levels of PPE--ranging from gloves only to fully encapsulated suits with onboard oxygen supply that require special training.
- Level A - Full Hazmat Suit,
- Level B - Chemical suit (for splashes),
- Level C - Firefighter gear (for inhalational protection).
- Level D - EMS uniform (no protection from chemical exposures)
After the Battle: Equipment Decontamination

Equipment decontamination is paramount to providing health and wellness, as well as for patient safety and reduced chance for transmission of infectious diseases. Sadly, equipment decontamination often is overlooked in the field.
Equipment should be fully decontaminated with the proper cleaning materials in the proper manner anytime exposure to body fluid occurs or after transport and treatment of a patient with a known infectious disease or symptoms consistent with an infectious disease that has yet to be diagnosed.
At the very least, even if there are no body fluids excreted nor any known infectious disease or symptoms of an infectious disease that has yet to be diagnosed, a clean sheet should be applied to the stretcher before each new patient.